Dysphagia Documentation Using OmniFlow® and Synchrony OmnisEMG™

OmniFlow® Breathing Therapy Biofeedback System and Synchrony Dysphagia Solutions by ACP® including OmnisEMG™ can be used in the treatment of patients with dysphagia. These devices provide interactive virtual reality biofeedback exercises to address underlying impairments. The use of specialized technology should be included in treatment documentation.
In clinical practice, documentation helps therapists communicate the treatment of a patient to other therapists and healthcare professionals. It also helps establish what treatment was performed to support proper billing claims for skilled services. Strong documentation conveys information in the six key areas defined below.
- CPT Code: Identify the services provided and billed.
- Underlying Impairments: Incorporate impairments (e.g., dyspnea, muscle fatigue, abnormal respiratory-swallow pattern) and their impact on functional performance (e.g., swallowing, phonation).
- Therapy Tests & Measures: Include appropriate patient-specific objective tests/measures and vital signs.
- Intervention/Technical Preparation: Identify exercise type performed and respective parameters to indicate change or progress in plan of care (e.g., repetitions/sets performed, volume level required). Include any special set-up or positioning needed.
- Skilled Therapeutic Interaction: Document how exercise and vital sign responses (before, during, and after a mode of treatment) were used to guide/adjust the treatment (e.g., SpO2 decreased to 89% and patient was given a 4-minute rest break, exercise resumed upon SpO2 96%). Include amount of verbal and tactile cues used.
- Client Performance: Periodically repeat the same tests/measures and vital signs and compare to previous/baseline values in order to assess progress, or lack thereof. Also document patient response to treatment and participation in therapy and facility activities.
OmniFlow® Breathing Therapy Biofeedback


Deep inhalation
(Diamond Mine)

Rhythmical breathing
(Starry Road)

Controlled expiration
(Sail Away)
Forced expiration
(Prehistoric Contest)

ACBT/Huffing technique
(The Dandelion)
Dysphagia Documentation Long-term Goal:
“Patient will improve respiratory-swallow pattern as evidenced by consumption of ≥ 75% of his regular diet within 30 minutes without oral residue, no report of complications, and with Dyspnea Scale decrease from 6/10 to 3/10 in 4 wks.”
Dysphagia (Respiratory-Swallow Cycle)
| CPT Code | “Session included controlled expiration and dysphagia treatment…” |
| Underlying Impairments | “…to address abnormal breathing patterns/expiratory volume to coordinate breathing/swallowing functions.” |
| Test & Measures | “Prior to treatment initiation, Dyspnea Scale = 6/10, SpO2 via pulse oximetry = 90%, HR = 80 bpm, RR = 20 breaths/min. Patient on 2L/min supplemental O2 via nasal cannula.” |
| Intervention/Technical Preparation | “Breathing therapy virtual reality biofeedback utilized for controlled expiration to support coordination of respiration-swallow cycle. Patient instructed to take a deep breath in, then exhale with breathing device set on easy level for 5 repetitions. This was followed by typical swallow intervention using sEMG virtual reality biofeedback with 10 second rest cycle and 2 second work cycle coordinating expiration before and after swallow during the work cycle.” |
| Skilled Therapeutic Interaction | “Therapist provided 2 verbal cues for proper breathing pattern with breathing exercise device. Therapist added typical swallow exercise using sEMG device to the treatment plan to assist with breathing-swallowing coordination.” |
| Client Performance | “Immediately following exercise vital signs were: SpO2 = 92% on room air, HR = 86 bpm, RR = 28 breaths/min, Dyspnea Scale = 4/10. Patient coordinated breathing on 17/25 swallows using a 5 ml thin liquid bolus compared to 13/25 on last session.” |
Synchrony OmnisEMG®

Kangaroo
Diver

Bow and Arrow
Trace Display
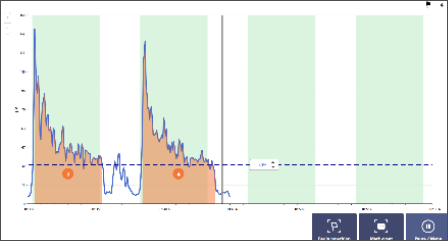
Work/Rest
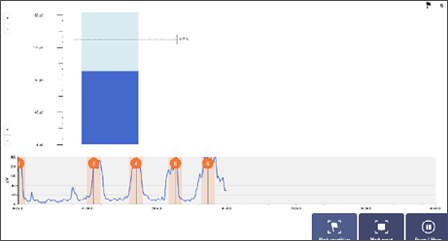
Bar Graph
Dysphagia Documentation Long-term Goal:
- “Patient will consume a regular diet with thin liquids without respiratory complications, weight loss, or dehydration in 4 wks.”
Dysphagia (Effortful Swallow)
| CPT Code | “Session included dysphagia treatment with effortful swallow exercise…” |
| Underlying Impairments | “…to address impaired base of tongue retraction, laryngeal elevation, and pharyngeal constriction.” |
| Test & Measures | “At evaluation, MASA score 140/200 indicating moderate dysphagia; MBSS results showing decreased base of tongue retraction, laryngeal elevation, and pharyngeal constriction causing pharyngeal wall residue and aspiration with thin and moderately thick liquids.” |
| Intervention/Technical Preparation | “sEMG virtual reality biofeedback utilized with 150% effort of his typical swallow on 62/75 swallows with a 5ml bolus of thin liquid. Effortful swallows performed to improve base of tongue retraction, laryngeal elevation, and pharyngeal constriction to decrease pharyngeal residue and occurrence of aspiration.” |
| Skilled Therapeutic Interaction | “Therapist provided verbal cues throughout session for patient to emphasize tongue to palate push. Due to patient’s improvements, therapist utilized thin liquid bolus this session from moderately thick in prior session.” |
| Client Performance | “Today’s session indicated an improvement of patient performing effortful swallows at 150% of typical swallow compared to 135% effort on last session and MASA score of 171/200 indicating mild dysphagia.” |
Featured Clinical Programs
Authors:
Andreé Akst, PT, MPT, CEEAA, NASM-CES, Clinical Services Content Specialist
Valerie Middleton, MA CCC-SLP, Clinical Program Consultant
CS-NEWS
Latest Updates
Subscribe to stay up-to-date on our latest posts.



