A 64-year-old long-term care resident was referred to therapy following an exacerbation of chronic heart failure that left her significantly weakened and with a marked decline in functional mobility. She lost her ability to independently propel her wheelchair and was also battling a non-healing, full-thickness pressure wound at the base of her spine, despite more than a month of standard wound care. To get her back on track, her care team turned to OmniVersa and OmniCycle.
Therapy Protocol
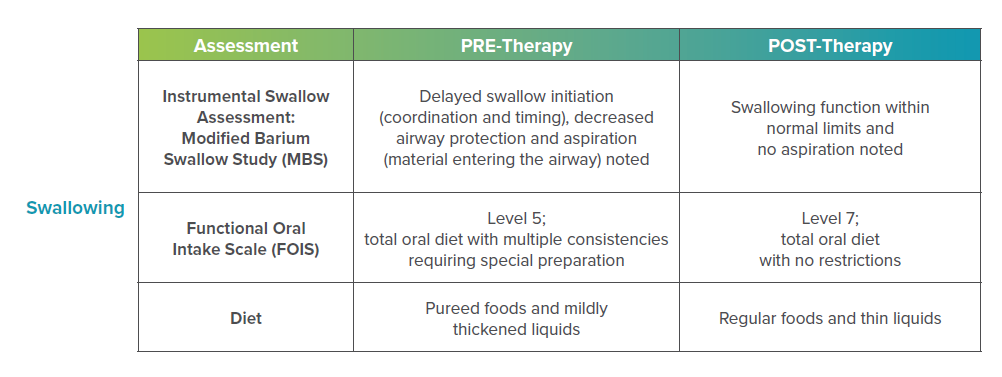
Speech Therapy
- 3-5x/week x 12 weeks
OmniVersa® Ultrasound/Electrotherapy System
- Subthermal ultrasound over the wound bed to increase local circulation and facilitate wound healing
OmniCycle® Elite Therapeutic Exercise System
- Upper and lower extremity cycling for improved strength and endurance
Additional Interventions
- Therapeutic exercise, self-care management, and wheelchair mobility training
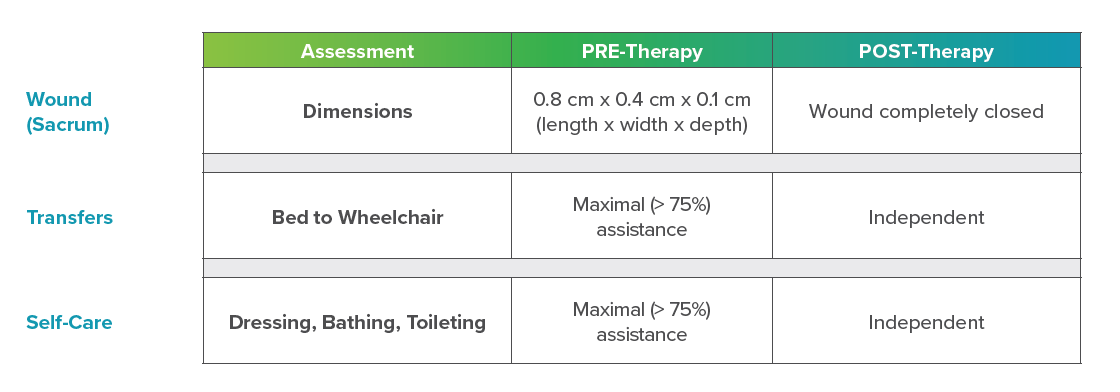
This patient was pleased with her progress in therapy. Since the wound has healed, she has regained independence with mobility and self-care. She is looking forward to relocating to Florida to be near her sister.
Explore ACP Technologies
With unmatched reliability, maximum treatment efficacy, and built-in safety features, you can trust ACP’s technologies to help your therapy team deliver the best possible patient outcomes.
MRK-BLOG-039
A 64-year-old long-term care resident was referred to therapy following an exacerbation of chronic heart failure that left her significantly weakened and with a marked decline in functional mobility. She lost her ability to independently propel her wheelchair and was also battling a non-healing, full-thickness pressure wound at the base of her spine, despite more than a month of standard wound care. To get her back on track, her care team turned to OmniVersa and OmniCycle.