Assisted living (AL) and independent living (IL) communities have made meaningful investments in wellness programming over the years. From group fitness classes to on-site therapy services, many residents are well supported. And yet, a large resident population continues to fall through the cracks. These residents live in what we call the wellness gap.
The wellness gap includes residents who don’t meet the criteria for skilled therapy services but are vulnerable to decline. They may be unable to participate in more traditional fitness programs like Zumba, yet still need supportive movement to maintain strength, balance, cognition, and independence. This group is larger than many operators realize, and it represents one of the most important and addressable opportunities for senior living communities today.
Why the Wellness Gap Matters
Residents in the wellness gap are often stable on paper, but they also aren’t building or maintaining the functional strength and mobility needed to age confidently in place.
This leads to predictable outcomes: weakness, increased fall risk, social withdrawal, and eventual transitions to higher levels of care. This progression impacts not only resident well-being, but also length of stay, care costs, and the ability to deliver on a promised wellness experience.
Where Traditional Wellness Programs Fall Short
Many wellness programs are unintentionally designed for residents who are already active, confident movers. Group classes like walking clubs or aerobics can feel intimidating, and limited staffing often makes it difficult to provide individualized support. As a result, residents in the wellness gap disengage—not because they don’t care about their health, but because the available programming doesn’t meet them where they are. To effectively support this population, communities need wellness solutions that are approachable, engaging, and adaptable across a wide range of abilities.
Closing the Gap with Technology
This is where immersive wellness technology plays a critical role. ACP provides wellness solutions designed specifically for older adults that support gentle, approachable movement.
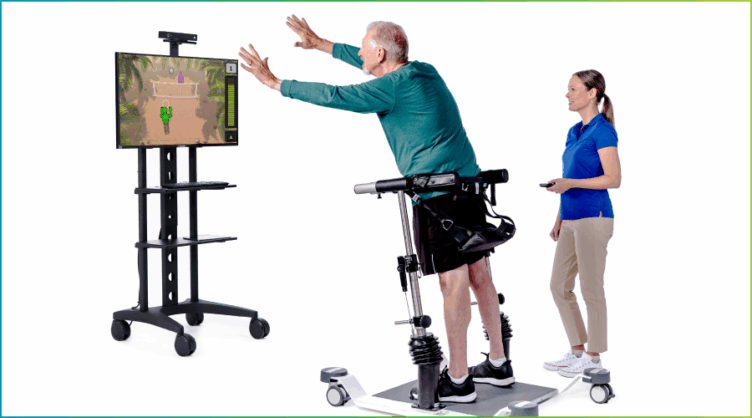
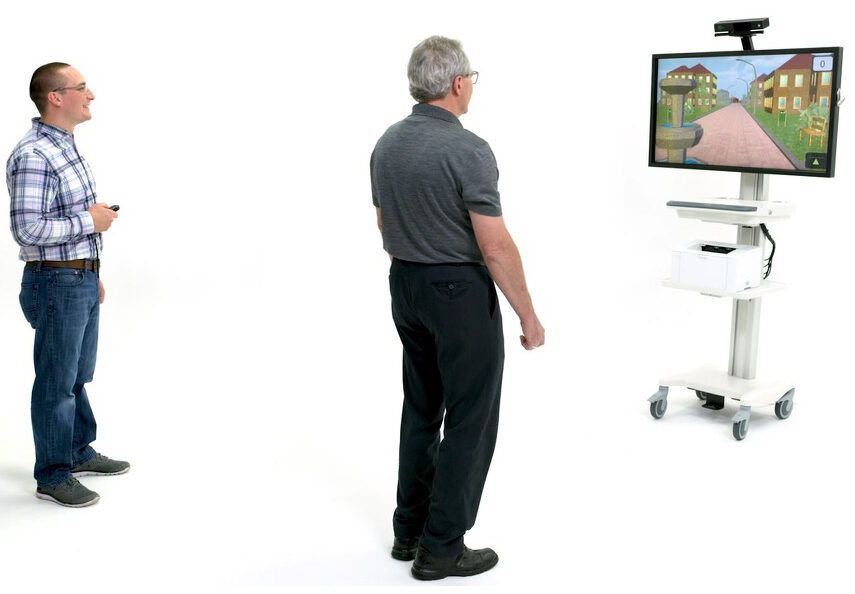
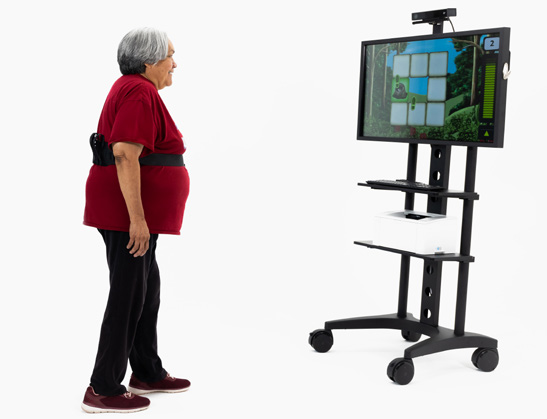
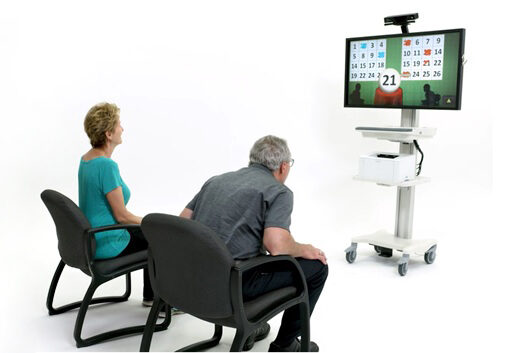
For residents in the wellness gap, tech-enabled experiences can be especially effective. Solutions like OmniVR® use game-inspired activities to support balance, coordination, strength, and cognitive engagement. With OmniTour™, routine cycling becomes an immersive journey that allows residents of all abilities to explore the world while exercising safely. Because these activities feel more like play than traditional exercise, residents who may otherwise opt out are far more likely to participate.
Drive Better Outcomes
By acting proactively, operators can intervene before decline sets in. When residents engage in regular, meaningful movement, communities can help:
- Reduce fall risk and prevent avoidable hospitalizations
- Support cognitive health and social connection
- Slow transitions to higher levels of care
- Demonstrate real wellness value to residents and families
In a competitive market, these outcomes matter. Prospective residents and families want communities that offer more than amenities and take a proactive, inclusive approach to healthy aging.
A More Inclusive Vision of Wellness
Wellness programs shouldn’t only serve the most active residents or those who qualify for therapy. The true measure of success is how well a community supports everyone. By investing in accessible, engaging wellness technologies, AL/IL communities can close the wellness gap, strengthen outcomes, and reinforce their commitment to helping residents thrive in place.
Wellness Solutions for Active Aging
Discover how ACP’s wellness technologies can support your community.
MRK-BLOG-037
Assisted living (AL) and independent living (IL) communities have made meaningful investments in wellness programming over the years. From group fitness classes to on-site therapy services, many residents are well supported. And yet, a large resident population continues to fall through the cracks. These residents live in what we call the wellness gap.